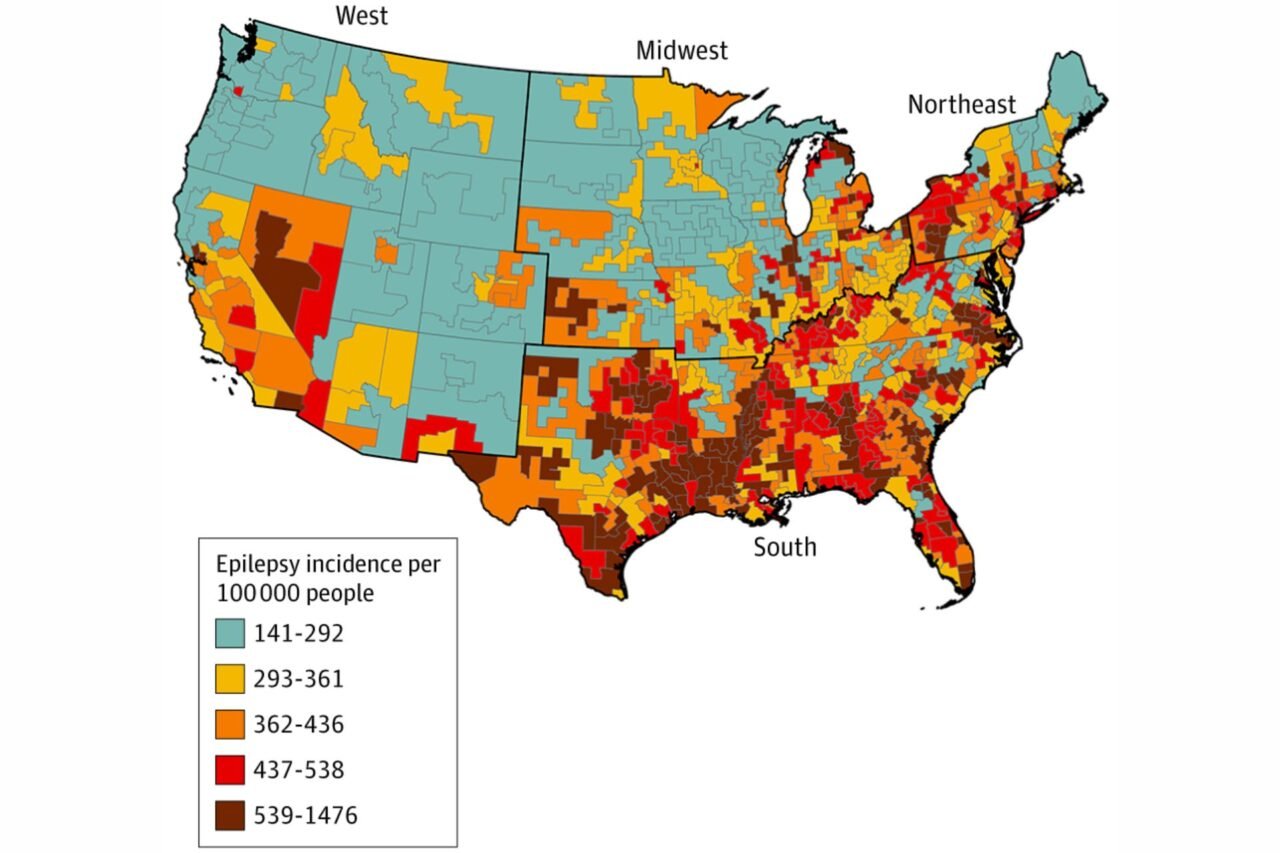
Research from the Houston Methodist Research Institute and Case Western Reserve University has revealed significant geographic disparities in epilepsy rates among older adults in the United States. The study, published in JAMA Neurology in March 2024, analyzed Medicare data from 2016 to 2019 and found that the southeastern U.S. exhibits notably higher rates of newly diagnosed epilepsy compared to other regions.
The investigation focused on approximately 20,000 cases diagnosed in individuals aged 65 and older in 2019. The southeastern states, particularly Louisiana, Mississippi, and Texas, reported the highest incidence rates. This emerging pattern suggests that specific risk factors related to these areas may contribute to the prevalence of this neurological disorder.
Understanding the Epilepsy Belt
Epilepsy is characterized by abnormal electrical activity in the brain, leading to recurring seizures. While the condition can have various causes, older adults are particularly susceptible. Previous studies indicated regional differences in diagnosed epilepsy cases, but this latest research is the first to map epilepsy incidence nationally among older Americans.
The researchers identified several factors correlated with the higher epilepsy rates in the “epilepsy belt.” For instance, insufficient sleep was more common in states like Louisiana, Alabama, and Georgia. Additionally, these southern states experienced a greater number of days with extreme heat, defined as a heat index above 95 degrees Fahrenheit, which may exacerbate health issues. Notably, states like Texas and Florida also reported higher rates of uninsurance, which can hinder timely medical intervention for younger residents, potentially delaying epilepsy diagnoses.
Siran Koroukian, a professor in the Department of Population and Quantitative Health Sciences at Case Western Reserve University, emphasized the significance of these findings. “This is the first study documenting such a strong association between extreme heat and incident epilepsy in older adults across the U.S.,” she stated. The implications of climate change on health, particularly as the population ages, are becoming increasingly relevant.
Broader Health Implications
The southeastern U.S. is also known for its elevated stroke rates, referred to as the “stroke belt.” Given that strokes are a major risk factor for developing epilepsy, it is likely that the intersection of these health issues plays a role in the increased incidence of epilepsy in this region.
Currently, approximately 3 million adults in the U.S. live with epilepsy. While there is no universal cure, effective treatments are available, including medications, surgery, and lifestyle adjustments to manage triggers. The researchers advocate for targeted public health interventions to address epilepsy prevention and care, particularly in regions with higher risks.
Strategies to consider include enhancing sleep quality, improving resilience to heat, and reducing barriers related to transportation and health insurance access. Such targeted approaches could significantly improve health outcomes for older adults susceptible to epilepsy in affected regions. The study’s authors assert that addressing these modifiable social and environmental conditions could guide future prevention efforts effectively.